Special task force for arrhythmia ablation
At the National Institute of Cardiology in Warsaw, nearly 1,000 heart arrhythmia ablation procedures are performed annually. Half of them are the most challenging procedures: performed on patients with a damaged heart and complex arrhythmias. Electrophysiologists Prof. Mariusz Pytkowski, MD, PhD, Michal M. Farkowski, MD, PhD and Aleksander Maciąg, MD, PhD, from the 2nd Department of Heart Arrhythmia at the National Institute of Cardiology in Warsaw talk about the treatment of the most complex cases.
Effective weapon
To effectively perform even the most demanding procedures, according to Prof. Mariusz Pytkowski, head of the 2nd Department of Heart Arrhythmia at the National Institute of Cardiology in Warsaw, one need: constantly updated and expanded knowledge, many years of experience and teamwork. As stated by the expert, a good organization of work and access to modern tools is no less critical.
– If during the ablation procedures of the most complex arrhythmias we would have at our disposal only an electrophysiological recorder and simple electrodes (this is classical electrophysiology), where we have no memory of the mapping electrode positioning or the possibility to create three-dimensional maps, the ablation procedure becomes much more complex and potentially less effective. Classical electrophysiology fails and does not provide sufficient facilities to carry out the most complex ablation therapies – emphasizes Prof. Mariusz Pytkowski.
Helping the critically ill
Transcatheter ablations in patients with structural heart disease are one of the most challenging types of procedures. Severely ill patients with damaged left ventricle (after heart attacks or with cardiomyopathies) usually have altered cardiac anatomy, and the sources of their arrhythmias are looked for in different places. 3D electroanatomical systems provide help with this.
– During endocardial ablation, we enter the inside of the heart from through veins or arteries. We operate with a catheter under fluoroscopy, which allows us to navigate the silhouette of the heart. We also use 3D electrophysiology systems that allow us to record electrical activation from inside the heart. The signals collected by the catheters are then received and displayed on the 3D electrophysiology system as a three-dimensional map of the heart cavities – explains Michal M. Farkowski, MD, PhD.
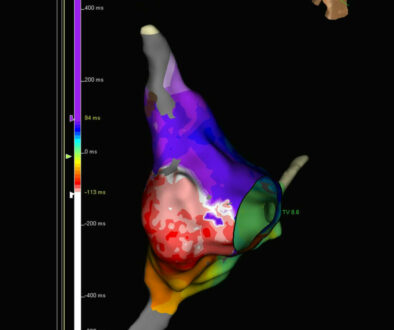
3D electroanatomical systems also allow assessment of the activation, shape, and magnitude of electrical potentials at a given location in the heart. Another function of these tools is the ability to create voltage maps of the heart.
– The voltage maps show us the voltages of the heart muscle tissue under the catheter-electrode at any given time. Throughout the procedure, we look for areas of reduced voltage as potentially being associated with arrhythmias. We also pay attention to any electrical diversity in the myocardium. The more fragmented or stretched the electrical potentials at a given site, the greater the chance we are dealing with the source of the arrhythmia. Precise identification and then neutralization of the arrhythmia source is critical because the procedure aims to damage precisely only areas responsible for abnormal conduction of impulses in the heart. If we performed applications in other points, they could become new arrhythmia sources – explains Doctor Farkowski.
Rare procedures
In a small percentage of patients, the source of arrhythmia is located not inside the heart (endocardium), where the blood flows, but on the other side of the heart muscle – the epicardium, the outer surface of the heart. In this case, doctors need to access the source of the arrhythmia from the epicardium to perform the ablation successfully. The so-called epicardial access is also preferred when the patient has a thrombus in the heart ventricle.
– Epicardial access begins with a puncture through the patient’s chest wall. The operator inserts a long needle and then an electrode near vital organs, such as liver, diaphragm, intestines, to reach the epicardial space. Finally, the electrode reaches the heart wall. Here the electrophysiologist must be careful with the delicate coronary vessels. For these reasons, the risk of complications in epicardial ablation is much higher than in endocardial ablation. I started to perform epicardial ablations after an almost year-long course and much training on simulators – says Doctor Maciąg.
To make the difficult procedure as effective as possible, electrophysiologists perform the ablation procedure using 3D maps of the heart cavities created by catheters for intracardiac and epicardial mapping. According to experts, modern catheters for “high-density” mapping are particularly useful here.
– The flat shape of the catheter itself, which we call a “fly swatter”, makes the electrode fit well in the pericardium and easy for the operator to use. Another advantage of this catheter is recording even several thousand mapping points from the pericardium (high density of recorded signals). The accuracy of a 3D map of heart cavities created based on much information is very high. It allows us to know precisely where we need to apply current to eliminate the arrhythmia effectively. In the most challenging cases, this can be critical to the effectiveness of the ablation procedure. The “high-density” mapping electrode is an example of an innovative solution that makes it possible to perform effective epicardial ablation, which would not have been possible a few years ago – explains Doctor Maciąg.
In centers with the highest referral level, where 300-500 arrhythmia ablation procedures are performed annually, epicardial ablations are performed several times a year. As confirmed by experts at the National Institute of Cardiology in Warsaw, the success rate of this procedure at leading electrophysiology centers is 60-80 percent and is comparable to endocardial ablations.